
The town of Butte, Montana, didn’t know what to make of Bobby.
The young man had always been restless. He dropped out of high school as a sophomore, and although everyone had thought he might skip town and roam, he’d gotten a job at Anaconda Mining Company. Everything had been fine for a little while, little mischiefs going unnoticed. Then, Bobby had been promoted to earth mover.
Then he’d driven the earth mover into the primary powerline for Butte. With a crackle, the city found itself in the dark for hours.
Police chases, stunts, thefts and less than legal money-making plots involving a hockey team would follow, earning him the nickname “Evel” because it rhymed with his last name, “Knievel.” Over the course of his life, he would break 433 bones and become one of the best-known daredevils in history. He would earn a title from the Guinness Book of World Records as the man who broke the most bones in a lifetime.
Knievel had a seemingly endless bounceback. However, not even he could make it through a life with so much trauma free of consequences: He suffered debilitating back pain and contracted Hepatitis C from one of the multiple blood transfusions he had over time. Seemingly, though, Knieval could not die of broken bones. He died of the complications of diabetes and idiopathic pulmonary fibrosis in 2007.
Physicians have long thought they understood the process of how bones healed themselves. They would be set in place, the way the bone was supposed to heal, and then a protein called fibrin would fill in the space where the structure had been broken. Fibrin is produced when tissue damage causes bleeding, converting it from fibrinogen into a usable form, like a clot. Those fibrin threads coagulated to form long chains entangled with blood. It has been said that bones are more vascular than many other structures in the body, and it may be true. They are designed to be full of blood.
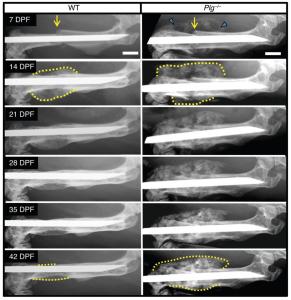
However, a new study published in the Journal of Clinical Investigation offers a little more insight on how the process of fracture repair works. The researchers, studying bone fractures in mice, found that mice whose bones healed normally lacked fibrinogen. In previous work, they noted that blood cells form first, followed by bone, contrary to previous thought.
Therefore, any condition associated with thrombosis (the act of clotting) or vascular disease impedes bone formation. Blood cell generation (angiogenesis) is more important to bone formation than anyone previously guessed.
Instead, fibrinogen itself is not the key to bone formation— the removal of fibrinogen is. If that removal is impaired, fracture repair will be slowed. This finding lines up with observations from chronic conditions such as diabetes, smoking, obesity and old age, where bone repair is slower and not as strong as before a break. Children’s bones also repair themselves more quickly after a fracture, which may be connected to the fact that children’s fibrin levels are approximately half that of adults.
Removal of fibrin is also essential for the prevention of heterotopic ossification, the development of bone in muscle due to fibrin threads being deposited between muscle fibers. It often results as an after-effect of osteopathic surgery and can be extremely painful and difficult to remove.
A better understanding of how bone fracture heals is important as we begin to live longer. In 2014, the National Osteoporosis Foundation estimated that 54 million American adults were affected by osteoporosis or low bone mass, which can lead to splintering and fracturing in bones. As we begin to live longer, it is more likely that we will develop low bone mass or osteoporosis. If we can understand better the process of how bone forms and heals itself, we can treat the condition better and make our quality of life better in the long-term.
Unless you’re Evel Knievel. In that case, you should probably get some better padding and plan for a life with a lot of downtime for broken bones sooner than later.
